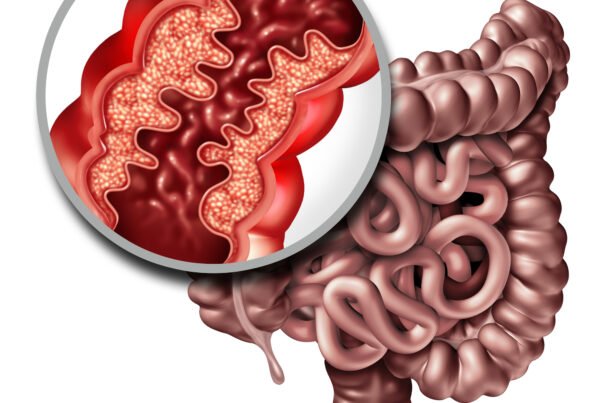
Understanding Crohn’s Disease – An Overview
December 24, 2021
Understanding Crohn’s Disease – An Overview
Sometimes referred to as Ileitis, Crohn's disease is a chronic condition known to cause inflammation…








Recent Comments